The “best medicine” is usually movement, not a pill.

If you’ve been dealing with aching knees, stiff hips, or cranky hands, you’ve probably been told to “take something for it.” Fair enough. But experts are now saying the best medicine for most chronic joint pain is rarely just an oral pain pill. It’s a plan.
Most arthritis pain improves most when you combine structured movement, weight management, and localized anti-inflammatory options like topical treatments, tailored to the joint that’s actually causing trouble.
1. Walking becomes your daily joint lubricant.

If there’s one habit that keeps joints from locking up, it’s simple, consistent walking. It’s not about speed or steps-per-day bragging rights. It’s about keeping cartilage nourished, muscles awake, and stiffness from setting up camp in your knees and hips.
The key is consistency and pacing. Ten minutes after breakfast, ten after dinner, and you’ve quietly built a pain-fighting routine without punishing your joints. This “boring” habit is a first-line treatment in major guidelines for osteoarthritis, which says a lot.
2. Strength training protects the joint by supporting it.

Most joint pain isn’t just about the joint. It’s about what’s failing to support the joint. Weak glutes make knees angry. Weak quads make stairs feel personal. Weak shoulders make reaching overhead feel like a betrayal.
A small strength routine, done two to three times a week, can reduce pain because it changes the load your joint absorbs. You stop relying on worn-down structures and start distributing force through muscle again. That’s why strength work is considered core treatment for knee and hip arthritis, not optional.
3. Water exercise lets you work hard without the backlash.

Water workouts are the closest thing to cheating in the best possible way. You can move more, bend more, and strengthen more without the sharp impact that makes joints flare up later. The buoyancy reduces stress, but the resistance still builds strength.
If you’re the type who wants to feel like you actually did something, water walking and water aerobics are surprisingly effective. Studies keep showing hydrotherapy helps pain and mobility in knee osteoarthritis, and it doesn’t come with the stomach and heart risks of daily pills.
4. Tai chi improves joint pain by training your balance.

Tai chi looks gentle, but it works like physical therapy dressed up as graceful movement. It builds control, balance, and strength in a way your joints tolerate well. For older adults, this matters because joint pain and instability are a dangerous combo.
The quiet benefit is that tai chi teaches your body to stop bracing and clenching through movement. When you move with less panic, you reduce strain. It’s consistently recommended in osteoarthritis guidelines because it lowers pain and improves function, with very low downside risk.
5. Weight loss helps even when it’s not dramatic.

Weight loss gets treated like it only counts if it’s a huge transformation. For joint pain, that’s not true. Even modest weight reduction lowers load through the knees and hips, which can reduce pain and improve function. You don’t need a “new body,” just less pressure.
It’s also not purely mechanical. Fat tissue can contribute to inflammation, which matters in arthritis. Experts now treat weight management like a core therapy, not a side suggestion, especially when paired with exercise and education-based self-management programs.
6. Topical diclofenac is often the first medication worth trying.
If one joint is screaming louder than the others, experts often prefer a localized fix. Topical NSAIDs like diclofenac gel can provide pain relief similar to oral NSAIDs, with fewer whole-body side effects. That matters more at 67 than it did at 47.
Think of it like treating the problem where it lives. You’re not bathing your stomach, kidneys, and cardiovascular system in anti-inflammatories just to calm one knee. Many people start with something like Voltaren and realize they didn’t need to escalate to pills at all.
7. Oral NSAIDs can work, but the long-term tradeoff is real.

Ibuprofen, naproxen, and celecoxib can be incredibly effective, and I’m not here to pretend they don’t help. But chronic use gets riskier with age, especially for GI bleeding, kidney injury, and cardiovascular issues. That’s why experts increasingly treat them as add-ons, not the main plan.
If you do use them, the smartest strategy is usually the lowest effective dose for the shortest time, and ideally not as a daily lifestyle. Pain relief is great, but not if you’re borrowing trouble from your future self.
8. Knee braces and canes are not “giving up.”

A brace or cane can feel like a public announcement that you’re officially old now. It isn’t. It’s a tool that changes mechanics and reduces pain, which makes you more active, which then improves pain further. That loop is what you want.
A large analysis found options like knee bracing and supports can be among the most effective non-drug treatments for knee osteoarthritis, helping pain and mobility. The best part is you can try them quickly, adjust easily, and feel the difference without waiting months.
9. Physical therapy works because it’s personal, not generic.
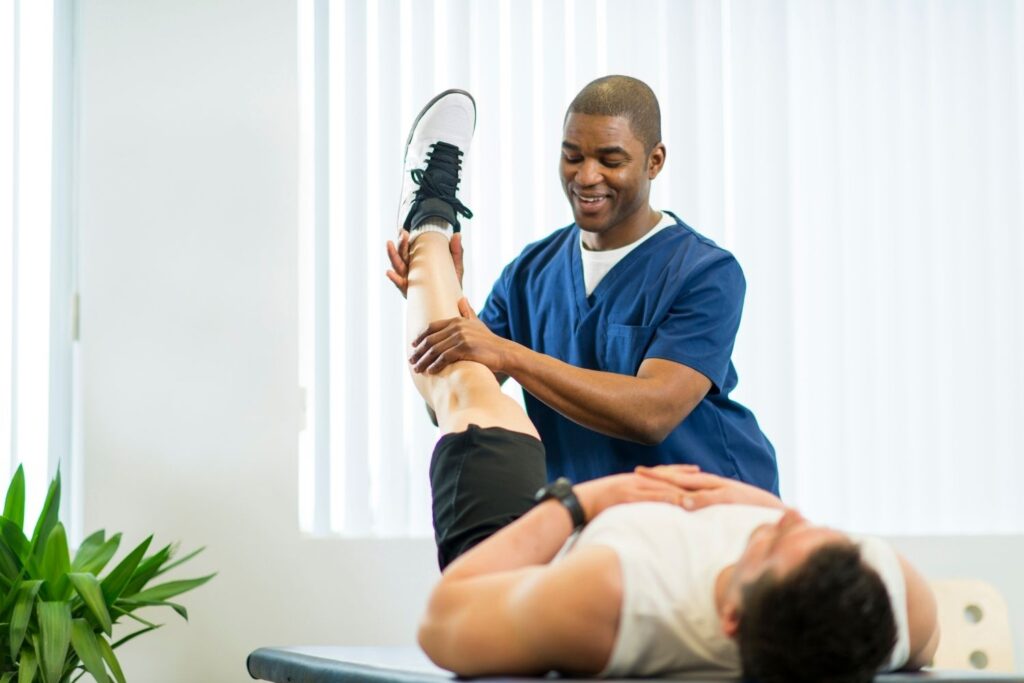
The reason physical therapy beats random workouts is that it matches your body. It targets what’s weak, tight, or compensating, and it teaches you how to move without irritating the same joint over and over. The right exercises feel boring until you realize you hurt less.
For example, knee pain might actually be a hip stability problem. Shoulder pain might be a posture and scapular control problem. A targeted plan stops the cycle of flare-ups. It’s not magic. It’s just precision, which is what most joint pain needs.
10. Education and self-management stop the pain flare spiral.

This part sounds unexciting, but it’s sneaky powerful. Knowing how to pace activity, modify movements, and recognize flare patterns can keep chronic joint pain from turning into a constant crisis. Education-based programs are now considered core treatment, not fluff.
When people feel helpless, they either avoid movement or overdo it on good days and pay for it later. Self-management helps you stay steady. A steady approach wins with arthritis because your joints respond best to consistency, not punishment or total rest.
11. The best plan is joint-specific, not one-size-fits-all.

A sore knee doesn’t need the same strategy as a sore shoulder, and neither should be treated like back pain. Experts emphasize tailoring treatment to the joint involved, because the mechanics and best supports differ. That’s why “just take pain meds” is such a weak plan by itself.
For focal pain in the knee, hand, or shoulder, a topical option may be your safest first move. For hip or knee arthritis, movement and strength are the foundation. The smartest plan is usually a mix, adjusted to your body, not a generic routine.
